Mental health and the journey to parenthood: Kristy's story
A very different experience with baby no.2
“I have struggled with anxiety throughout my life, so before I had my first baby I was really nervous about how I would feel. In the end, everything was fine, and I had a healthy pregnancy.
But with my second baby, I had a very tough time.
I developed hyperemesis gravidarum at around six weeks and was being sick every day. It became so bad that at eight weeks I had to go to hospital because I had severe dehydration.
It affected my mood straight away.
People tell you to enjoy the time before the baby comes, but instead of ‘blooming’ I was constantly sick.
I couldn’t enjoy my pregnancy or spend any quality time with my two-year old. I also found that people didn’t understand the difference between morning sickness and hyperemesis.
People would say ‘Well I had morning sickness too, just have a ginger biscuit.’ Or when I would go to the pharmacist, they would tell me I shouldn’t be taking medication because I was pregnant. It felt like a constant battle having to explain that my GP had prescribed it and that the relatively unknown risks of taking this medication whilst pregnant was not as big as the risks associated with severe dehydration.”
Fighting for a home birth
“Midway through my pregnancy I also developed obstetric cholestasis - a liver condition, which made my skin incredibly itchy. Risks of this condition are also stillbirth and haemorrhage after birth.
I had planned to have a home birth and was really excited about it, but the hospital consultant told me I couldn’t have one because of my condition and that I would likely need to be induced.
As I only had mild obstetric cholestasis, I researched the risks of having a home birth with my husband and decided that it was better to stick to our original plan than be induced.
Our home birth midwives were fully supportive of our choice, but despite this my consultant still wanted to induce me.
At one point towards the end of my pregnancy I felt like I was at hospital every day for three weeks, arguing with consultants, registrars and hospital midwives that the decision I was making was right for us, and that the risks associated with forced induction outweighed the risks of mild obstetric cholestasis.
I didn’t want to be induced unless it was absolutely necessary; I wasn’t ready, and the baby wasn’t ready to be born.
The consultant made me write a statement saying that I understood what she was saying and that I was happy to put my baby’s life at risk.
Aside from being incredibly distressing for me, this was also against the hospital guidelines concerning women who have obstetric cholestasis and we later put in a formal complaint, supported by our home birth midwives.
I was very emotional at the time and because my husband was working he couldn’t attend every appointment with me. It sat with me for such a long time, as soon as I signed it I felt sick. It was awful.
At the same time, my home birth midwives were continually testing my blood to check I was safe to remain at home. At 39 weeks we found out my bile acid levels had increased to the boundary of our ‘safe’ line and was told that unless I went into labour that evening, I would need to go to hospital in the morning to be induced. I was happy to be induced if it was medically necessary, although it made me very nervous.
Luckily, I went into labour that night and had a healthy baby boy, at home, as we had planned.”
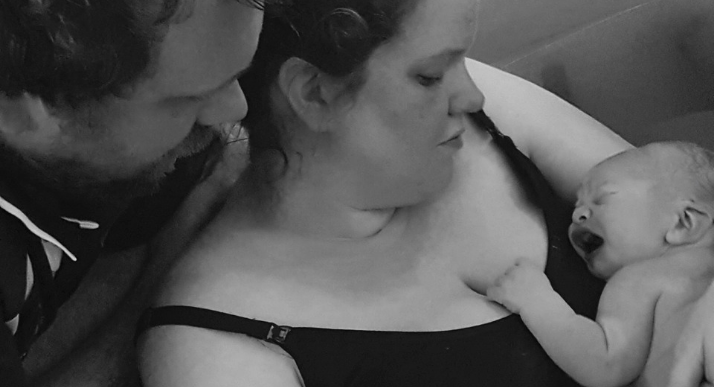
Back to hospital
“After the illness I had experienced through pregnancy I expected to be fine once I had given birth, but I soon developed acute mastitis within a week of having my son. This caused my breasts to be very sore and meant I couldn’t feed without screaming in agony.
Just five days after my son was born I went to hospital where I was told me to go home with painkillers for a migraine.
My home birth midwife, on the other hand, checked my blood test results later, called me at home and sent me straight to the GP. The GP was shocked at the stage of my mastitis and noticing all signs of sepsis I was rushed back to hospital, where I was pumped full of antibiotics very quickly.”
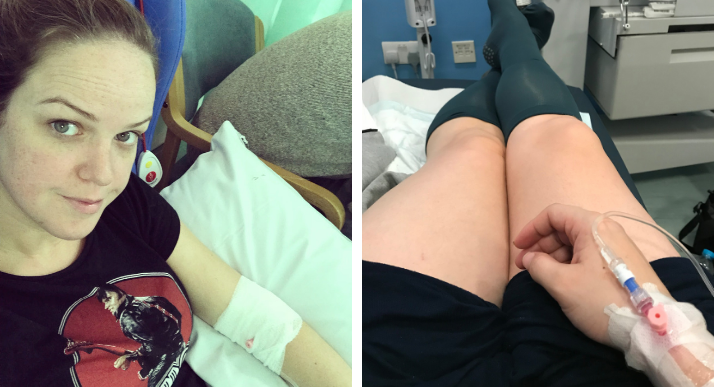
Feeling pressured
“I was admitted to hospital, feeling incredibly unwell. During my stay there staff began making comments that I had two sons. They would say things like, ‘I bet you’re disappointed’ and ‘Oh well, you can try again for a girl next.’
I hadn’t given much thought to the gender balance of my family, but I suddenly started looking at my new son and thinking maybe you’re not meant for me, you’re not my child, I’m meant to have a girl. My mind was increasingly running away with thoughts I couldn’t control.
I ended up discharging myself after a few days even though I was still really poorly. I couldn’t get any rest in the hospital, I felt so stressed that I couldn’t be with my children and I was sick of comments about having two boys.”
Feeling like a failure
“After being at home for a week, I got the symptoms of mastitis again. Every time my baby made a noise I started to have a panic attack because I knew I had to try and feed him.
I’ve always felt huge pressure to breastfeed, as it’s so drilled into you that ‘breast is best.’ I would try and feed him whilst biting my arm to get through the pain and slowly I started to resent him. I was terrified every time he woke up because I knew he’d be hungry.
One day, during a visit from my home birth midwife, I had a complete meltdown. I couldn’t breastfeed anymore – I felt like I would rather die. Along with my midwife and my husband we made the decision to stop breastfeeding. I was already taking a high dose of antibiotics for mastitis, so I stopped cold turkey.
After stopping, there were 48 hours where I felt like I was being electrocuted. I was biting pillows all night in pain, it was horrific.
I was really emotional and struggling to bond with my son, but of course no one could even give me a hug because the pain was so intense. It was like being stabbed a thousand times in both breasts with a million tiny swords.
I fell into this feeling of failure. I’ve failed to breastfeed. I’ve failed to have a girl. I’ve failed to create the perfect family.
I looked at my son and felt like I didn't recognise him. I really felt my children would be better off without me.
Several times I wondered things like ‘how much could I hurt myself if I threw myself out of the top window?’ It felt like I’d fallen through the floor and was being swallowed by the earth. I was drowning.”
Feeling thankful for some support
“The home birth midwives were meant to discharge me after 10 days but they kept coming for another three weeks. They could see how much pain I was in and decided to refer me to the perinatal mental health team.
Within 10 weeks I had my first appointment and started having weekly sessions until just before my son’s first birthday.
Without the care of my home birth midwives, I wouldn’t have gone to the GP about my mental health - their support was vital to my recovery. My husband and I truly believe the attention and care they gave me may have saved my life.”
Talking about how I was feeling
“I didn’t recognise I was ill, I just thought I had failed, that the boys deserved a better mother, and I thought everything would be better once I was physically well. I was so ashamed to talk about how I was feeling, because we’re told how lucky we are to have a baby.
I felt I couldn’t admit ‘I’m a bit sad that I haven’t got a daughter,’ - something I never thought I’d be sad about until the reaction from both friends and strangers on the set up of my family.
It wasn’t until my sixth therapy session that I asked my therapist if what I was experiencing was postnatal depression, and I finally accepted it.
This made me feel relieved. I wasn’t a bad mum, I was very unwell.
My psychiatrist helped me through cognitive behavioural therapy. We talked a lot about my past, as well as looking at ways to deal with my unrealistic expectations of trying to be the ‘perfect’ mum.
She taught me about thinking errors and we worked through different ways to approach situations that triggered my anxiety and depression. I still use them now, every day.”
Have you been affected by this story?
If the content of this story causes you to think of anything that has happened to you or someone you know and you feel upset, worried or uncomfortable, please see the Maternal Mental Health Alliance's support page for a list of services who may be able to help.


